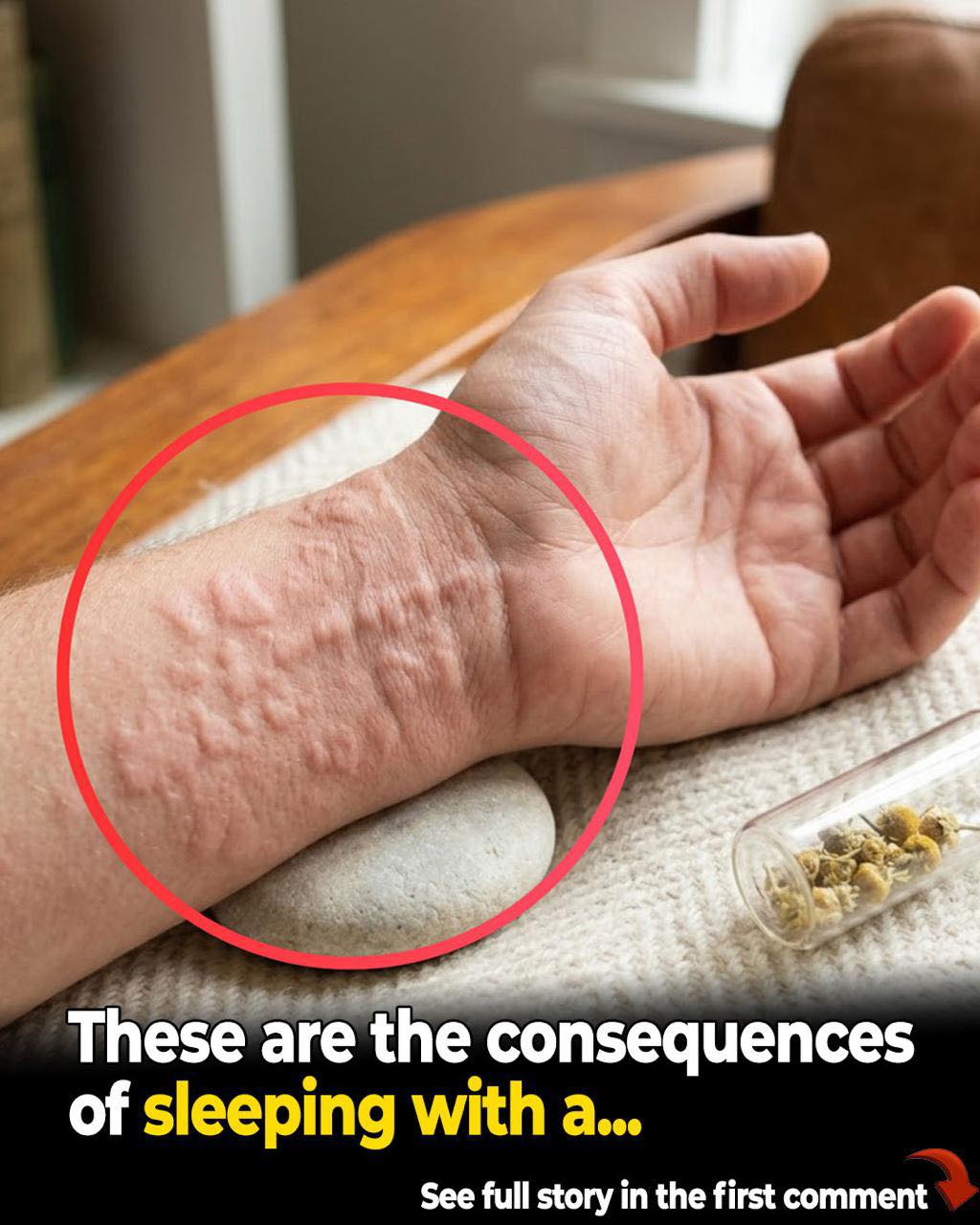
Hives can seem random because they erupt fast, move fast, and often vanish before anyone else sees them. One welt may itch hard, swell, sting, or burn, then flatten within hours. Yet the skin is usually reacting to something real, even when the trigger stays hidden at first. ACAAI lists foods, medications, infections, latex, pressure, cold, heat, exercise, and sun exposure among known causes.
That range explains why people often blame the wrong thing. A shrimp dinner gets blamed, while the true trigger was a cold, ibuprofen, a tight waistband, or a hot shower. The American Academy of Dermatology also names stress, sunlight, scratching, and pressure as possible triggers. For chronic hives, the cause may stay unclear, and some cases are linked to immune or thyroid problems.
Acute hives last less than 6 weeks. Chronic hives last longer and may recur for months or years. Either form needs urgent care when swelling affects the mouth, face, or throat, or when breathing becomes difficult. These 8 overlooked hive triggers can explain repeated outbreaks and show which details deserve closer attention. A good trigger hunt looks at timing, setting, symptoms, and repeat exposure. That wider view often reveals what the skin has been trying to say.
Infections Can Trigger Hives Even When Allergy Seems More Likely

Many people blame hives on the last thing they ate, then ignore the cold that started 2 days earlier. That instinct is understandable, yet it often sends the search in the wrong direction. The American Academy of Allergy, Asthma and Immunology says viral infections are the “most common” cause of acute urticaria. AAAAI also lists viral illness among the leading triggers. That means a sore throat, cough, stomach virus, or lingering congestion may matter more than lunch. When the immune system reacts to an infection, histamine can surge and produce raised, itchy welts. The skin then becomes the visible part of an immune response. That is why hives sometimes arrive before the real culprit is obvious.
Bacterial illness can do the same. AAAAI lists urinary tract infections and strep throat as recognized triggers. DermNet also includes dental abscesses, sinusitis, and mycoplasma. Those causes are easy to miss because they do not always peak beside the rash. A person may have mild throat pain, a tender tooth, or sinus pressure, yet focus only on the sudden welts. AAD also notes that infections can trigger hives. It names strep throat, a urinary tract infection, and COVID-19 as examples. The outbreak may therefore look like an allergy when it is actually part of the body’s defense system.
Timing often provides the clearest clue. Hives may begin during a cold. They may also show up as other symptoms are fading. In some cases, they appear after an infection seems mostly gone. That delay makes people suspicious of dinner, detergent, or stress instead. Acute hives also move quickly. One welt may fade within hours while another appears somewhere else, which adds to the sense of mystery. Yet a recent infection can still fit the picture. When hives follow fever, cough, diarrhea, sore throat, dental pain, or painful urination, the trigger hunt should widen immediately. The rash may need treatment, yet the surrounding illness deserves attention.
A practical review starts with the week before the outbreak. Think about colds, stomach bugs, sinus symptoms, dental problems, sick contacts, or urinary symptoms. Then match those details against the first day of hives and each later flare. Photographs also help because welts often vanish before a clinic visit. Write down any fever, fatigue, or body aches as well. If swelling affects the lips or tongue, or if breathing becomes difficult, urgent care is essential.
If hives keep returning after one illness ends, medical review is wise. A clinician can then sort whether another infection, a medicine, or chronic urticaria is involved. The key point is simple. A rash that looks random may actually be the skin’s response to an infection that seemed minor or unrelated. Sometimes the clue is a child’s cold. Other times it is a stubborn sinus problem. It may even be a tooth that has started throbbing. When those details line up with the welts, the mystery shrinks. That is not glamorous detective work, yet it often points toward the cause faster than guessing about meals.
Common Painkillers and Antibiotics Can Be the Hidden Cause
People expect hives from an unusual drug, not from a familiar tablet they have taken for years. Yet common medicines are among the most overlooked triggers. ACAAI lists antibiotics, aspirin, and ibuprofen among frequent causes. DermNet says drug-induced urticaria often involves penicillin, NSAIDs, or sulfa combinations. Because these medications are ordinary, the connection is easy to miss. The rash gets blamed on food, pollen, or stress while the actual trigger sits in a bathroom cabinet. That mistake is especially common when the medicine was taken for a headache, period pain, or a sore throat. A common pill can therefore hide in plain sight.
Painkillers deserve special attention because they can cause hives or worsen hives that already exist. AAAAI says that some patients will find that ibuprofen or aspirin will trigger hives. DermNet adds that nonsteroidal anti-inflammatory drugs can cause urticaria without classic immune activation. That detail counts because people often assume a reaction must follow one familiar allergy pathway. Sometimes the medicine still causes the rash, even when the mechanism is different. A person may take a painkiller after a hard day, wake with welts, and never suspect the tablets were involved. If the same pattern repeats, the clue becomes hard to ignore. The timing can be much louder than the packaging.
Antibiotics create another layer of confusion. When hives appear during treatment, the medicine may be responsible, yet the underlying infection may also be the trigger. That overlap is why timing becomes so important. A clinician will want to know when the medicine started. They will also ask how fast the rash appeared. They will ask whether swelling affected the lips, face, or throat. Reactions can occur early, late, or after many previous doses without trouble. No one should retest a suspected trigger at home when the earlier reaction was severe. Drug reactions can escalate quickly and may become dangerous. That is especially true when breathing symptoms join the rash.
The smartest move is to build a medication timeline. Include prescription drugs, painkillers, cold remedies, vitamins, herbal products, and topical treatments. Then compare that list with the first day of hives and each later flare. If welts repeatedly follow ibuprofen, aspirin, or a new antibiotic, that pattern deserves serious weight. Write down dose changes too. Also, note whether the rash improved after the medicine stopped. If breathing trouble, faintness, or throat tightness appear with the rash, emergency care is appropriate.
Drug allergies and drug-triggered hives can overlap with anaphylaxis, which requires immediate treatment. A familiar medicine may seem too ordinary to blame. Sometimes, however, the most routine pill in the house is the reason the skin keeps erupting. Save the bottle names. Record the dates. Note the start and stop times. Those details often reveal a pattern faster than memory alone in practice. They also help a clinician decide whether avoidance, substitution, or allergy testing makes sense. Without that record, people often blame the wrong exposure. They then repeat the same trigger during the next illness or pain flare.
Pressure, Scratching, and Tight Clothing Can Set the Skin Off

Not every hive starts with something swallowed or inhaled. Some begin where the skin is rubbed, scratched, or pressed. AAD explains that pressure from tight clothing, a purse strap, or scratching can trigger hives. For some people, the most common inducible form is dermatographism. AAD calls it “writing on the skin.” That phrase sounds playful, yet the reaction is real. A waistband, bra strap, shoulder bag, rough seam, or even a fingernail can set off swelling within minutes. Because scratching follows itching, the trigger and the reaction often reinforce each other.
Pressure can also work on a delay. DermNet says delayed pressure urticaria may appear 4 to 6 hours after a pressure event. Standing, walking, hard seats, or tight clothes can all set it off. That delay makes the cause easy to miss. Someone may blame dinner or detergent because the rash started in the evening. The true trigger may have been the belt, backpack, or chair from much earlier in the day. This form can also produce deeper swelling and tenderness, not only surface welts. The body map often gives the best clue. Hives that track the beltline, shoulders, feet, or buttocks point strongly toward pressure.
The NHS lists “scratching or pressing on your skin” as a trigger. That helps explain why this form is often overlooked. People expect an allergy to enter the body first. In many cases, the problem begins with force on the skin itself. Location helps here. Linear welts, strap-shaped swelling, and outbreaks under snug clothing all support a physical trigger. Timing helps as well. If a rash rises where skin was rubbed, then fades, that pattern is useful. It becomes even stronger when the same friction sets it off again. Those details help separate pressure hives from eczema, contact dermatitis, or insect bites.
Relief often starts with practical changes. Looser clothing, smoother fabrics, softer seams, and less friction can lower the number of flares. Fast treatment of itching also helps because scratching can create more welts. Photos are worth taking before the rash fades. So are notes about what touched the skin earlier that day. If outbreaks become painful, last longer, or involve deeper swelling, medical review is wise. Pressure hives are not always simple, and in some cases, they coexist with chronic urticaria. Still, many unexplained outbreaks stop looking mysterious once clothes, straps, seats, and skin friction enter the picture.
Watchbands can matter too. So can sports straps, shapewear, and firm shoe edges. Long car rides may leave clues on the back or thighs. A heavy grocery bag can irritate one shoulder but not the other. Those small details may look trivial. In practice, they often explain why hives seem to choose the same spots. Once that pattern is visible, daily habits become easier to adjust. Keeping a simple note on clothing, straps, exercise, and sitting time can make a hidden trigger visible. It also prevents endless guessing about meals, pollen, or skin care. Pressure hives may be stubborn, yet they are often far from random.
Heat, Sweat, Exercise, and Stress Can Spark Cholinergic Hives

Some hives appear when body temperature rises, not when a new substance enters the body. That idea surprises many people because heat seems too ordinary to cause a rash. DermNet describes cholinergic urticaria as hives triggered by stimuli that induce sweating. It even lists “Exercise (most common trigger)” in plain terms. Hot baths, spicy food, emotional stress, and warm rooms can also provoke this form. ACAAI adds that exercise, alcohol, and emotional stress may worsen itching. The body’s heat response, therefore, becomes the trigger, even when no outside allergen is involved. That is one reason these flares are often misread.
The appearance of the rash can help identify it. DermNet says cholinergic urticaria often produces small wheals that last 15 to 30 minutes. They may begin on the chest, neck, or upper body, then spread if the trigger continues. Someone may notice them after a jog, a fast walk in summer, a hot shower, or a tense event. Because the welts can fade quickly, the outbreak gets dismissed as simple overheating. That is why photos matter. Without them, the rash may be gone before a clinician sees it, and the history may sound vague. The size and short life of the wheals are often the clue.
Stress also needs a careful explanation. It should never be used as a lazy answer when the cause is uncertain. Still, AAD lists stress among recognized triggers. The NHS also includes emotional stress in situations that can produce hot, sweaty skin and hives. In this setting, stress is not a mystical explanation. It is part of a body process. That process raises temperature, increases sweating, and may release hives in people already prone to them. That distinction keeps the discussion grounded. It also stops the trigger search from turning into blame.
Pattern tracking is usually the most useful tool. Ask whether the rash appears after workouts, hot showers, crowded rooms, spicy meals, or tense situations. Notice whether cooling down helps it fade. Also note whether the welts are tiny and short-lived or larger and more persistent. Those details can distinguish cholinergic hives from heat rash, eczema, or contact irritation. A sudden flush before the wheals can matter too. So can itching that starts while exercise is still underway. If hives arrive with wheezing, abdominal pain, light-headedness, or heavy swelling, urgent care becomes important. Even common triggers deserve serious attention when symptoms spread beyond the skin.
For many people, repeated flares stop seeming random once heat, sweat, and body temperature enter the story. Some people also notice flares in steam rooms or after rushing for a train. Others react during emotionally charged events, then cool off and clear quickly. Those repeat scenes matter. They show that the trigger may be heat generation itself, not the soap, clothes, or outdoor air. Once that link is clear, prevention becomes far more practical. Short walks instead of hard runs may help during evaluation. So may cooler showers, lighter layers, and a pause before spicy meals on hot days.
Cold Air, Sunlight, and Water Can All Act as Hive Triggers

Weather and light rarely top the suspect list, yet they can trigger hives in the right person. ACAAI lists cold, heat, and sun exposure among physical stimuli that can cause urticaria. The NHS goes further and notes “water or sunlight, but this is rare.” Rare triggers still affect real patients. A person may break out after cold wind, a frozen drink, a pool, or bright sun. Because those situations seem harmless, the rash is often blamed on dry skin, chlorine, or ordinary irritation instead. That mistake can delay the right diagnosis for months. It can also make a true physical trigger look imaginary.
Cold urticaria deserves respect because it can become dangerous. DermNet says hives may develop after exposure to cold air, cold water, or cold objects. It also warns that swimming in cold water can lead to serious symptoms. ACAAI gives a similar warning about whole-body cooling. That means a rash after wind or a chilled drink is not always a small inconvenience. If large areas of skin react at once, the body can respond more broadly. Someone who notices cold-triggered welts should take pool or ocean reactions seriously. That is especially true when dizziness, faintness, or swelling appears.
Sun-triggered hives create a different kind of confusion. DermNet says solar urticaria can develop within minutes of sunlight exposure and often fades quickly after the exposure stops. That speed can make the rash look almost unreal. It may arrive before a sunburn would appear and vanish before anyone thinks to photograph it. Some people also assume that sunlight can only cause tanning or burning. In solar urticaria, however, the skin produces swelling and itch instead. AAD notes that sunlight can trigger hives, and NHS guidance supports that point. Fast timing is the clue that separates hives from many other sun-related rashes.
The best practical approach combines caution with observation. Note whether welts rise after cold wind, cold drinks, swimming, showers, or direct sun. Watch how quickly they appear and how fast they settle. That timing helps distinguish hives from irritation or dryness. Protective clothing and trigger avoidance can reduce flares while the cause is being sorted. For cold-triggered cases, sudden swimming deserves extra caution because the reaction can spread fast. For sun-triggered cases, photos and careful timing help confirm the pattern. The main lesson is straightforward.
A trigger does not need to be eaten, inhaled, or applied from a bottle. Sometimes, the air, the temperature, the water, or the light itself is what sets the skin off. Thin clothing can mislead people, too. DermNet notes that solar urticaria may affect areas under light fabric, depending on the rays and the sheerness. That can make the rash seem random. A cool breeze can do the same. People may only notice the welts during rewarming, not at the coldest moment. Those details are small, yet they often explain why a physical trigger stayed hidden. Once timing, temperature, and exposure line up, these odd-looking flares usually start making much more clinical sense overall.
Food Is a Real Trigger, but Additives and Alcohol Can Distort the Picture

Food absolutely can cause hives, and sometimes it causes a dangerous allergic reaction. Yet food is also blamed far more often than it deserves. ACAAI lists peanuts, eggs, nuts, and shellfish among common food triggers for acute hives. That guidance becomes strongest when hives follow the same food more than once. Still, AAAAI puts it plainly, calling additives “rarely a cause” of hives. It also says chronic hives are rarely due to an allergy. Those points help explain why many people cut major foods, then watch the rash return anyway. A strong suspicion is not the same as a repeatable trigger.
Additives and alcohol complicate the picture further. AAAAI notes that annatto yellow dye and carmine are known exceptions among additives. It also says alcohol and spices may worsen urticaria, although the evidence is low. That means a glass of wine may not create the whole problem. It can still make an existing flare itch harder or spread further. People often confuse worsening with causation. They also forget about sauces, colorants, gelatin, mixers, protein powders, and restaurant ingredients. When the timeline is vague, blame lands on the entire meal instead of the one component that mattered.
The strongest clue is repeat timing. True food-triggered hives usually follow exposure in a consistent way. A person eats shrimp, peanuts, or another culprit, then develops symptoms again after eating it later. The window may be minutes to several hours, depending on the trigger. AAAAI says that when there is a direct cause and effect with food, you usually notice it within that period. Random daily flares over many weeks fit less neatly with classic food allergy. That is why endless elimination diets often create stress without solving the rash. A focused diary usually helps more than a long list of forbidden foods.
Precision becomes most important when symptoms move beyond the skin. Hives with vomiting, wheezing, hoarseness, throat tightness, dizziness, or faintness need urgent care. Food allergy can escalate quickly, and ACAAI lists those symptoms among the signs of anaphylaxis. Outside emergencies, the goal is to identify repeatable triggers without turning eating into a guessing game. Write down the exact foods, drinks, sauces, supplements, and timing of each episode. Include alcohol, because it may intensify a flare even when it is not the sole cause. Food can absolutely explain hives. It just should not dominate every case by default.
In many stubborn outbreaks, the bigger answer lies with medication, infection, pressure, temperature, or the immune system itself. Restaurant meals create special confusion because sauces and garnishes hide the details. Shared fryers can also muddy the picture. So can dessert toppings and drink mixers. That is why a written record helps more than memory. Record the meal, the time, the first symptom, and whether the same food caused trouble before. If the pattern never repeats, food becomes less convincing. If the same item sparks welts twice, suspicion rises fast. That disciplined approach prevents panic and keeps the trigger hunt anchored to evidence instead of fear alone.